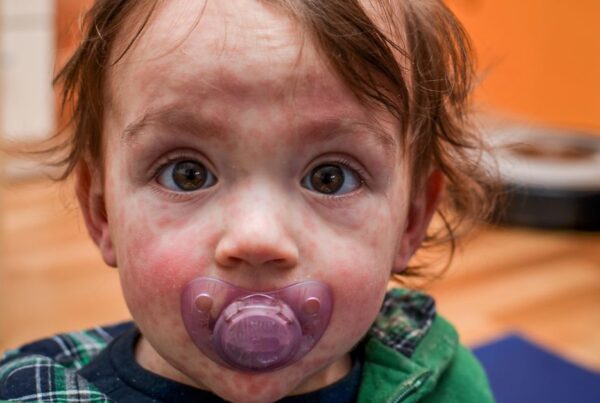
Eczema is an inflammatory skin condition that affects up to 25% of children. Eczema is known for its symptoms of red, itchy, dry, and sometimes painful skin. Babies are especially prone to eczema because of their delicate skin barrier, which causes their skin to be more sensitive to allergens and other skin irritants. Because it is so common, many parents have asked me to write about integrative eczema treatment.
There are several different types of eczema, but atopic dermatitis is the most common and that’s what we’ll be covering in this article. Other types of eczema include contact dermatitis, dyshidrotic eczema, hand eczema, neurodermatitis, nummular eczema, and stasis dermatitis. We’ll cover the treatment of these other types of eczema in future articles. However, the basic principles of managing flares, improving skin health, and reducing inflammation hold true for any integrative eczema treatment plan.
What Is Eczema?
Eczema is a complex inflammatory skin condition. Skin-barrier damaging inflammation results from an overactive immune system. The damaged skin barrier loses water quickly making it dry, itchy, and more sensitive to irritation. Eczema patches appear red in light skin tones and purple, brown, or gray in darker skin tones.
Though eczema isn’t contagious and doesn’t lead to serious life-threatening disease, it can have a significant negative effect on quality of life and should always be treated with care.
What Are The Symptoms of Eczema?
Eczema symptoms typically start in infancy or childhood, though they can begin later in some. Eczema is a chronic condition and children may grow out of it or they may continue to experience flares throughout their lives.
Eczema is known for the characteristic dry, itchy rash which can be red, purple, brown, or gray depending on the underlying skin tone. People with eczema may also experience dry, cracked skin; small, raised bumps; and skin that oozes and crusts. Continued scratching can lead to raw, sensitive skin; increased susceptibility to skin infections; and thickened skin, known as lichenification.

Why Does The Immune System Become Imbalanced?
The immune system is our internal surveillance system. It needs to recognize and remove invaders while sparing our own cells. The immune system is incredibly complex and every year we understand more about it. However, for this article, we will focus on one small part: the TH2 cells.
TH2 cells are also called T-Helper cells. Their job is to respond to environmental cues and secrete messenger molecules, called cytokines, which increase inflammation and recruit a strong immune response. When working well, TH2 cells keep us safe from bacteria, parasites, and toxins. When in overdrive, TH2 cells react to things that aren’t a threat like pollen, gluten, etc, and contribute to the development of allergic conditions like eczema, asthma, and food allergies.
We don’t know why some people get stuck in an overactive TH2 response, and the causes are most likely multifactorial. Some hypotheses include:
- Hygiene hypothesis: reduced exposure to bacteria and parasites due to our overly sanitized world leads to an under-stimulated and hyper-responsive immune system.
- Glutathione depletion: experimentally, glutathione depletion can lead to a TH2 dominant immune response. Things that lead to glutathione depletion include oxidative stress (eg from poor diet, lack of exercise, mercury/thimerosal toxicity post-vaccination, medications like acetaminophen, infections, some chronic diseases, etc.) and certain genetic mutations that impact the body’s ability to make glutathione.
- Micronutrient status: iron, zinc, and selenium; vitamins A, D, E, C, B6, and B12; and folic acid are particularly important in maintaining immune system function and flexibility.
- Aluminum exposure: stimulates the TH2 immune response.
- Microbiome imbalance: the healthy bacteria that live in our gut, skin, and lungs play an important role in balancing our immune system, and a disturbed microbiome is strongly correlated with allergy. This likely explains why children born via cesarean section are more likely than children born via vaginal delivery to develop eczema. This might also be why some parents find that topical application of antibacterial agents like colloidal silver help reduce symptoms associated with eczema.
- Impaired skin barrier proteins: it’s known that many people with eczema have genetic mutations that reduce the efficacy of the skin barrier. This leaves them with more sensitive skin, which is more prone to dryness and the development of allergic conditions.
- Genetics and epigenetics
Being familiar with the possible causes allows us to create eczema treatment plans that don’t just focus on reducing symptoms, but also on the underlying causes.
Read more about glutathione: Taking Tylenol? The Glutathione Connection – Dr. Green Mom
Note: the immune system involvement in allergies and eczema is much more complex than simply overactive TH2 cells, but as far as we understand right now, TH2 cells play a dominant role.
Eczema Treatment
An integrative approach to eczema treatment focuses on soothing the skin and providing comfort during flares, reducing the body’s inflammatory burden, creating a healthy microbiome, improving overall skin health, and balancing the immune system.
Acute Treatment of Eczema Flares
It is important to manage acute eczema flares, especially if they cause discomfort or itching. This is to provide symptom relief, but also to prevent chronic scratching that can lead to infections and/or thickening of the skin.
My first course of action is to use a gentle and thick moisturizing balm that also contains botanical anti-inflammatories. For most people, these balms work quickly to reduce symptoms. However, it is important to know that a small subset of people with eczema who are in a very allergic state will develop allergies to any plant-based moisturizer. When I have one of these patients in my practice, I might resort to vaseline as a moisturizer. Though I try to stay away from petroleum products, this is one case where the petroleum base is actually a benefit because allergies to vaseline are extremely rare. I really like Henry’s Homestead healing salve for reducing inflammation and relieving itch.
If a moisturizer along with the systemic treatments discussed below don’t provide enough relief to stop scratching and allow the skin to heal, then I consider a short-term topical corticosteroid treatment. Corticosteroids come with a lot of side effects, but they are sometimes the best option to control symptoms while working on the root causes.

Reducing Inflammatory Burden
Inflammation accompanies allergic disease. If the body is already in a highly inflamed state, then allergic reactions tend to be worse. Lifestyle is the most important modifiable factor for decreasing inflammation and is an important part of holistic eczema treatment.
Lifestyle changes that decrease inflammation include the following:
- Spending time outside: a minimum of 30 minutes per day if possible
- Getting good sleep and having regular sleep and wake times
- Eating an anti-inflammatory diet
- Avoiding food allergens
- Being mindful of your toxic burden
- Spending time doing things you love with people you love
- Reducing stress
- Increasing omega 3 fatty acid intake
Read more:
- Basics Of An Anti-Inflammatory Lifestyle
- 10 Ways To Support Detoxification In Kids
- Stress Relief For Kids
- 21 Different Types Of Food Sensitivities
- Reasons Your Kids Aren’t Sleeping (And How To Help)
Improving The Health of The Gut & Microbiome
Improving the health of the gut and microbiome can help treat eczema. When we think of microbiome health, probiotics are the first thing that comes to mind. Indeed, probiotics have a demonstrated benefit for microbiome improvement and eczema treatment. However, creating an optimal microbiome involves more than just taking probiotics!
One of the most important things you can do for a healthy microbiome is to eat a diverse diet including vegetables and legumes, fermented foods, polyphenol-rich foods, and prebiotic foods. Infants should be breastfed for the first six months or more if possible. Non-breastfed infants may benefit from the addition of a probiotic to their formula.
Exercise, time in nature, hormone health, and stress all impact the microbiome as well. Playing outside in the sunshine is the easiest way to improve all of those things!
Read more about healing the gut: How To Heal The Gut (For Kids)
Improving Overall Skin Health
Taking care of the skin from the inside and outside is important for good skin health. To care for skin, stay hydrated, eat brightly colored fruits and vegetables (especially yellow and orange ones), and choose hypoallergenic skin products, cleaners, and clothing detergents without synthetic fragrance.
It is important not to over-bathe as this can strip oils from the skin. A 10-15 minute daily bath or shower in warm, not hot, water is recommended, followed by the application of a moisturizer within 3 minutes to seal in hydration. Use a gentle cleanser instead of harsh soap, and avoid scrubbing affected areas. Pat skin dry rather than rubbing with a towel.
For babies under a year old, bathing advice changes based on whether or not the baby has eczema. For babies without eczema, it is recommended not to bathe them more than once per week. Each additional bath per week increases the risk of developing eczema. However, for babies with eczema, a daily bath is recommended to keep the skin clean and reduce the risk of developing an infection. Be sure to moisturize after the bath to keep the skin hydrated.
Read more about healing baths here:

Immunomodulators For Eczema Treatment
Immunomodulating treatment involves balancing the immune system. There are both natural and conventional approaches to immunomodulation.
Natural approaches include plant sterols and sterolins, medicinal mushrooms, and immunomodulating herbs. These medicines tend to have far-reaching positive effects on the immune system, the endocrine system, and the body as a whole. Probiotics and omega 3 supplements may also be able to help rebalance the immune system through their interaction with the gut microbiome. Natural immune rebalancing treatments tend to take a long time to work, so you have to stick with them.
It’s essential to identify and remove food allergies so that the immune system isn’t constantly activated. I usually recommend an elimination diet for identification of food allergies for adults and older kids, however IgE and IgG testing may be a more realistic approach for young kids and babies. It’s important to be aware that not every person who has eczema also has food allergies. The most common allergens associated with eczema are eggs and dairy, but gluten, soy, corn, strawberry, and citrus all deserve mentions as well.
Conventional immunomodulating treatments include topicals like tacrolimus, pimecrolimus, and crisaborole, as well as systemic medications like dupilumab and tralokinumab. These may come with serious side effects, so they should be a last option. Speak with your doctor for more information.
Eczema Prevention
Eczema is best prevented in the prenatal period when the immune system is being programmed. There is evidence that when moms supplement with fish oil, probiotics, and vitamin D, their babies may have a reduced chance of developing eczema.
When it comes to giving babies supplements to prevent the development of eczema, results are less clear. However, exposure to sunlight does seem to have a protective effect. Just be sure to enjoy sunshine responsibly and watch out for burns.
Daily use of moisturizers doesn’t reduce the chances of developing eczema, but limiting bathing to once per week does. However, if eczema is present, daily baths with moisturizers are recommended as described above.
Summary
Eczema is an inflammatory skin disease that is a result of complex interactions between the skin barrier and the immune system. Symptom management is just as important as getting to the root cause. An integrative approach to eczema treatment may include both natural and conventional interventions as needed.
References:
Chalmers, J. R., Haines, R. H., Bradshaw, L. E., Montgomery, A. A., Thomas, K. S., Brown, S. J., Ridd, M. J., Lawton, S., Simpson, E. L., Cork, M. J., Sach, T. H., Flohr, C., Mitchell, E. J., Swinden, R., Tarr, S., Davies-Jones, S., Jay, N., Kelleher, M. M., Perkin, M. R., Boyle, R. J., … BEEP study team (2020). Daily emollient during infancy for prevention of eczema: the BEEP randomised controlled trial. Lancet (London, England), 395(10228), 962–972. https://doi.org/10.1016/S0140-6736(19)32984-8
Cabana, M. D., McKean, M., Caughey, A. B., Fong, L., Lynch, S., Wong, A., Leong, R., Boushey, H. A., & Hilton, J. F. (2017). Early Probiotic Supplementation for Eczema and Asthma Prevention: A Randomized Controlled Trial. Pediatrics, 140(3), e20163000. https://doi.org/10.1542/peds.2016-3000
Bigman G. (2020). The Relationship of Breastfeeding and Infant Eczema: The Role of Reverse Causation. Breastfeeding medicine : the official journal of the Academy of Breastfeeding Medicine, 15(2), 114–116. https://doi.org/10.1089/bfm.2019.0269
Maslin, D., Veitch, D., & Williams, H. C. (2020). Direct infant ultraviolet light exposure is associated with eczema and immune development: a critical appraisal. The British journal of dermatology, 182(2), 300–303. https://doi.org/10.1111/bjd.18087
Rueter, K., Jones, A. P., Siafarikas, A., Chivers, P., Prescott, S. L., & Palmer, D. J. (2021). The Influence of Sunlight Exposure and Sun Protecting Behaviours on Allergic Outcomes in Early Childhood. International journal of environmental research and public health, 18(10), 5429. https://doi.org/10.3390/ijerph18105429
Szari, S., & Quinn, J. A. (2019). Supporting a Healthy Microbiome for the Primary Prevention of Eczema. Clinical reviews in allergy & immunology, 57(2), 286–293. https://doi.org/10.1007/s12016-019-08758-5
Rautava, S., Kainonen, E., Salminen, S., & Isolauri, E. (2012). Maternal probiotic supplementation during pregnancy and breast-feeding reduces the risk of eczema in the infant. The Journal of allergy and clinical immunology, 130(6), 1355–1360. https://doi.org/10.1016/j.jaci.2012.09.003
Sun, M., Luo, J., Liu, H., Xi, Y., & Lin, Q. (2021). Can Mixed Strains of Lactobacillus and Bifidobacterium Reduce Eczema in Infants under Three Years of Age? A Meta-Analysis. Nutrients, 13(5), 1461. https://doi.org/10.3390/nu13051461
Xiong, Z., Zhou, L., Chen, Y., Wang, J., Zhao, L., Li, M., Chen, I., Krewski, D., Wen, S. W., & Xie, R. H. (2022). Prevalence of eczema between cesarean-born and vaginal-born infants within 1 year of age: a systematic review and meta-analysis. European journal of pediatrics, 181(6), 2237–2247. https://doi.org/10.1007/s00431-022-04436-5
Baron, R., Taye, M., der Vaart, I. B., Ujčič-Voortman, J., Szajewska, H., Seidell, J. C., & Verhoeff, A. (2020). The relationship of prenatal antibiotic exposure and infant antibiotic administration with childhood allergies: a systematic review. BMC pediatrics, 20(1), 312. https://doi.org/10.1186/s12887-020-02042-8
Williams, H. C., & Chalmers, J. (2020). Prevention of Atopic Dermatitis. Acta dermato-venereologica, 100(12), adv00166. https://doi.org/10.2340/00015555-3516
Trikamjee, T., Comberiati, P., D’Auria, E., Peroni, D., & Zuccotti, G. V. (2021). Nutritional Factors in the Prevention of Atopic Dermatitis in Children. Frontiers in pediatrics, 8, 577413. https://doi.org/10.3389/fped.2020.577413
Hon, K. L., Tsang, Y. C., Pong, N. H., Lee, V. W., Luk, N. M., Chow, C. M., & Leung, T. F. (2015). Patient acceptability, efficacy, and skin biophysiology of a cream and cleanser containing lipid complex with shea butter extract versus a ceramide product for eczema. Hong Kong medical journal = Xianggang yi xue za zhi, 21(5), 417–425. https://doi.org/10.12809/hkmj144472
Luschkova, D., Zeiser, K., Ludwig, A., & Traidl-Hoffmann, C. (2021). Atopic eczema is an environmental disease. Allergologie select, 5, 244–250. https://doi.org/10.5414/ALX02258E
Zeiser, K., Hammel, G., Kirchberger, I., & Traidl-Hoffmann, C. (2021). Social and psychosocial effects on atopic eczema symptom severity – a scoping review of observational studies published from 1989 to 2019. Journal of the European Academy of Dermatology and Venereology : JEADV, 35(4), 835–843. https://doi.org/10.1111/jdv.16950
Greer, F. R., Sicherer, S. H., Burks, A. W., COMMITTEE ON NUTRITION, & SECTION ON ALLERGY AND IMMUNOLOGY (2019). The Effects of Early Nutritional Interventions on the Development of Atopic Disease in Infants and Children: The Role of Maternal Dietary Restriction, Breastfeeding, Hydrolyzed Formulas, and Timing of Introduction of Allergenic Complementary Foods. Pediatrics, 143(4), e20190281. https://doi.org/10.1542/peds.2019-0281
Böhm, I., & Bauer, R. (1997). Th1-Zellen, Th2-Zellen und atopische Dermatitis [Th1 cells, Th2 cells and atopic dermatitis]. Der Hautarzt; Zeitschrift fur Dermatologie, Venerologie, und verwandte Gebiete, 48(4), 223–227. https://doi.org/10.1007/s001050050573
Eyerich, K., & Novak, N. (2013). Immunology of atopic eczema: overcoming the Th1/Th2 paradigm. Allergy, 68(8), 974–982. https://doi.org/10.1111/all.12184
Biedermann, T., Skabytska, Y., Kaesler, S., & Volz, T. (2015). Regulation of T Cell Immunity in Atopic Dermatitis by Microbes: The Yin and Yang of Cutaneous Inflammation. Frontiers in immunology, 6, 353. https://doi.org/10.3389/fimmu.2015.00353
Walker, J., McKenzie, A. TH2 cell development and function. Nat Rev Immunol 18, 121–133 (2018). https://doi.org/10.1038/nri.2017.118
Peterson, J. D., Herzenberg, L. A., Vasquez, K., & Waltenbaugh, C. (1998). Glutathione levels in antigen-presenting cells modulate Th1 versus Th2 response patterns. Proceedings of the National Academy of Sciences of the United States of America, 95(6), 3071–3076. https://doi.org/10.1073/pnas.95.6.3071
James, S. J., Slikker, W., 3rd, Melnyk, S., New, E., Pogribna, M., & Jernigan, S. (2005). Thimerosal neurotoxicity is associated with glutathione depletion: protection with glutathione precursors. Neurotoxicology, 26(1), 1–8. https://doi.org/10.1016/j.neuro.2004.07.012
Elmadfa, I., & Meyer, A. L. (2019). The Role of the Status of Selected Micronutrients in Shaping the Immune Function. Endocrine, metabolic & immune disorders drug targets, 19(8), 1100–1115. https://doi.org/10.2174/1871530319666190529101816
Pascal, M., Perez-Gordo, M., Caballero, T., Escribese, M. M., Lopez Longo, M. N., Luengo, O., Manso, L., Matheu, V., Seoane, E., Zamorano, M., Labrador, M., & Mayorga, C. (2018). Microbiome and Allergic Diseases. Frontiers in immunology, 9, 1584. https://doi.org/10.3389/fimmu.2018.01584
Pfefferle, P. I., Keber, C. U., Cohen, R. M., & Garn, H. (2021). The Hygiene Hypothesis – Learning From but Not Living in the Past. Frontiers in immunology, 12, 635935. https://doi.org/10.3389/fimmu.2021.635935
Drislane, C., & Irvine, A. D. (2020). The role of filaggrin in atopic dermatitis and allergic disease. Annals of allergy, asthma & immunology : official publication of the American College of Allergy, Asthma, & Immunology, 124(1), 36–43. https://doi.org/10.1016/j.anai.2019.10.008
Heimall, J., & Spergel, J. M. (2012). Filaggrin mutations and atopy: consequences for future therapeutics. Expert review of clinical immunology, 8(2), 189–197. https://doi.org/10.1586/eci.11.100
Lin, T. K., Zhong, L., & Santiago, J. L. (2017). Anti-Inflammatory and Skin Barrier Repair Effects of Topical Application of Some Plant Oils. International journal of molecular sciences, 19(1), 70. https://doi.org/10.3390/ijms19010070
Lloyd-Price, J., Abu-Ali, G., & Huttenhower, C. (2016). The healthy human microbiome. Genome medicine, 8(1), 51. https://doi.org/10.1186/s13073-016-0307-y
Shanahan, F., Ghosh, T. S., & O’Toole, P. W. (2021). The Healthy Microbiome-What Is the Definition of a Healthy Gut Microbiome?. Gastroenterology, 160(2), 483–494. https://doi.org/10.1053/j.gastro.2020.09.057
Bathing frequency is associated with skin barrier dysfunction and atopic dermatitis at three months of age Marrs T., Perkin M.R., Logan K., Craven J., Radulovic S., McLean W.H.I., Versteeg S.A., (…), EAT Study Team (2020) Journal of Allergy and Clinical Immunology: In Practice, 8 (8) , pp. 2820-2822.
Bouic, P. J., & Lamprecht, J. H. (1999). Plant sterols and sterolins: a review of their immune-modulating properties. Alternative medicine review : a journal of clinical therapeutic, 4(3), 170–177.
El-Heis, S., D’Angelo, S., Curtis, E. M., Healy, E., Moon, R. J., Crozier, S. R., Inskip, H., Cooper, C., Harvey, N. C., Godfrey, K. M., & MAVIDOS Trial Group (2022). Maternal antenatal vitamin D supplementation and offspring risk of atopic eczema in the first 4 years of life: evidence from a randomized controlled trial. The British journal of dermatology, 187(5), 659–666. https://doi.org/10.1111/bjd.21721
Jensen-Jarolim E. (2015). Aluminium in Allergies and Allergen immunotherapy. The World Allergy Organization journal, 8(1), 7. https://doi.org/10.1186/s40413-015-0060-5