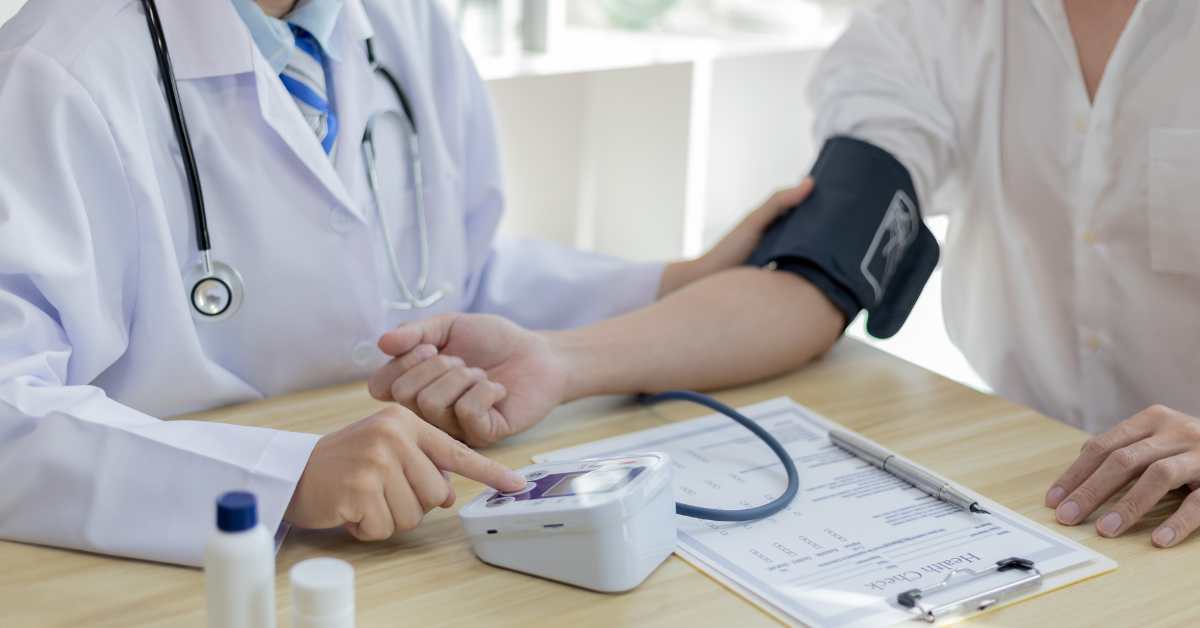
We’ve never had to worry about kiddos with high blood pressure. Unfortunately, today the risk factors for adult hypertension are the same for kids: obesity, sedentary lifestyle, poor nutrition, and genetic susceptibility.
We’ve never had to worry about kiddos with high blood pressure. Unfortunately, today the risk factors for adult hypertension are the same for kids: obesity, sedentary lifestyle, poor nutrition, and genetic susceptibility.
What is Pediatric Hypertension?
According the the Mayo Clinic:
- Hypertension is defined as average systolic blood pressure (SBP) and/or diastolic blood pressure (DBP) that is greater than or equal to the 95th percentile for sex, age, and height on three or more occasions.
- Prehypertension in children is defined as average SBP or DBP levels that are greater than or equal to the 90th percentile, but less than the 95th percentile.
- As with adults, adolescents with BP levels greater than or equal to 120/80 mmHg should be considered prehypertensive.
- A patient with BP levels above the 95th percentile in a physician’s office or clinic, who is normotensive outside a clinical setting, has white-coat hypertension. Ambulatory BP monitoring (ABPM) is usually required to make this diagnosis.
Conventional Medical Treatment
National Institutes of Health (NIH)-
Commonly Prescribed Medications
(please see NIH paper above for common dosages/age):
Angiotensin-converting enzyme (ACE) inhibitor
- Benazepril
- Captopril
- Enalapril
- Fosinopril
- Lisinopril
- Quinapril
Angiotensin-receptor blocker
- Irbesartan
- Losartan
Alpha and Beta- blocker
- Labetalol
Beta- blocker
- Atenolol
- Bisoprolo/HCTZ
- Metoprolol
- Propanolol
Calcium channel blocker
- Amlodipine
- Felodipine
- Isradipine
- Extended-release nifedipine
Central Alpha-agonist
- Clonidine
Diuretic
- HCTZ
- Chlorthalidone
- Furosemide
- Spironolactone
- Triamterene
- Amiloride
Peripheral Alpha-agonist
- Doxazosin
- Prazosin
- Terazosin
Vasodilator
- Hydralazine
- Minoxidil
Naturopathic Medical Treatment Options
(may be used in conjunction with conventional options and/or used alone)
Diet
- fruits and vegetables (dirty dozen/clean 15), whole grains, lean proteins, healthy fats
- remove excess salt, sugar and unhealthy fats from the diet
- fiber – psyllium husk, oats
Exercise (for weight related hypertension)
- PLAY, PLAY, PLAY
- engage in sport activities
- exercise should be FUN, please get creative for your child
- 30-60 minutes per day
Vitamins and Supplements
- Fish Oil- EPA + DHA = 1-2 grams per day with food
- Magnesium 200-400 mg daily
Other Options
- Arginine 1-2 grams daily (do NOT give if child is taking an ACE inhibitor)
- Sleep- 9-12 hours sleep per night (age dependent)
Resources:
The effect of a fibre supplement compared to a healthy diet on body composition, lipids, glucose, insulin and other metabolic syndrome risk factors in overweight and obese individuals. British Journal of Nutrition 2011; 105(1):90–100.
Giacosa A, Rondanelli M. The right fiber for the right disease: An update on the psyllium seed husk and the metabolic syndrome. Journal of Clinical Gastroenterology 2010; 44 Suppl KS58–S60.
Mori TA, Bao DQ, Burke V, et al. Docosahexaenoic acid but not eicosapentaenoic acid lowers ambulatory blood pressure and heart rate in humans. Hypertension 1999; 34(2):253–260.
Nelin LD, Hoffman GM. L-arginine infusion lowers blood pressure in children. Journal of Pediatrics 2001; 139(5):747–749.
Skowron, Jared M. (2011-08-02). 100 Natural Remedies for Your Child: The Complete Guide to Safe, Effective Treatments for Childhood’s Most Common Ailments, from Allergies to Weight Loss. Rodale.
Williams CL, Hayman LL, Daniels SR, Robinson TN, Steinberger J, Paridon S, et al. Cardiovascular health in childhood: A state- ment for health professionals from the Committee on Atherosclerosis, Hypertension, and Obesity in the Young (AHOY) of the Council on Cardiovascular Disease in the Young, American Heart Association. Circulation 2002;106:143–60.
Whelton SP, Chin A, Xin X, He J. Effect of aerobic exercise on blood pressure: A meta- analysis of randomized, controlled trials. Ann Intern Med 2002;136:493–503.
Robinson TN. Behavioural treatment of childhood and adolescent obesity. Int J Obes Relat Metab Disord, 1999;23 Suppl 2:S52–S57.
Barlow SE, Dietz WH. Obesity evaluation and treatment: Expert Committee recom- mendations. The Maternal and Child Health Bureau, Health Resources and Services Administration and the Department of Health and Human Services. Pediatrics 1998;102:e29. Available at: www.pediatrics.org/cgi/content/full/102/3/e29. Verified July 12, 2004.
Krebs NF, Jacobson MS. Prevention of pedi- atric overweight and obesity. Pediatrics 2003;112:424–30.
U.S. Department of Health and Human Services. The Surgeon General’s call to action to prevent and decrease overweight and obesity. Rockville, MD: U.S. Department of Health and Human Services, Public Health Service, Office of the Surgeon General. 2001.
Gutin B, Owens S. Role of exercise intervention in improving body fat distribution and risk profile in children. Am J Human Biol, 1999;11:237–47.
Siega-Riz AM, Popkin BM, Carson T. Trends in breakfast consumption for children in the United States from 1965–1991. Am J Clin Nutr 1998;67:748S–756S.
Warren JM, Henry CJ, Simonite V. Low glycemic index breakfasts and reduced food intake in preadolescent children. Pediatrics 2003;112:e414. Available at: www.pediatrics.org/cgi/content/full/112/ 5/e414. Verified July 12, 2004.
Reviewed/Updated: 09/14
Content Created: 05/14